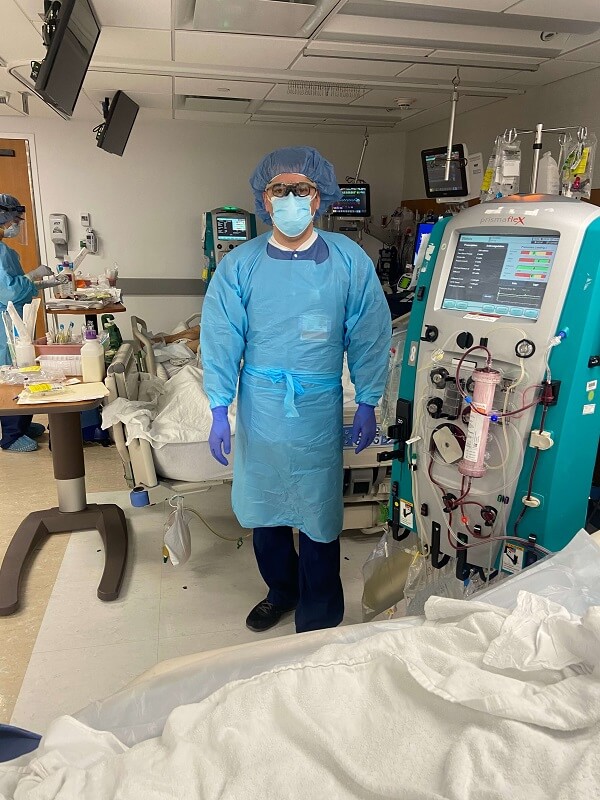
Omar Bholat, DDE ‘20
On March 1st, as the first cases of COVID-19 were discovered in New York, the physicians across Northwell Health began expanding capabilities to prepare for the pandemic. Northwell Health is the largest private healthcare system in the country and has extensive resources. However, there was just no way to fully expand readiness in such a constrained environment. The hospital had its disaster plan, with surge capacity for patients requiring intensive care. It had 97 beds in five Intensive Care Units (ICUs) and rapidly expanded capacity to accommodate more than 250 critically ill patients. As a surgeon, with expertise in trauma and critical care, I became part of the team caring for the most critically ill patients, under the most difficult conditions. With everything from PPE to nurses in short supply, we found a way to do more with what we had. As opposed to throwing away N95 masks after each use, they were re-used until no longer serviceable. While nurses usually care for one or two critically ill patients, they were routinely assigned three critical patients. My colleagues in surgery had all of their elective cases cancelled, received re-training from critical care physicians, and began taking care of complex patients with multi-system organ failure. Patients with adult respiratory distress syndrome required additional and critical strategies. Continuous dialysis was initiated as treatment for life threatening acidosis. Different medical regimens were employed to blunt the effects of COVID-19 on the body with varying success. The effects of this disease on the body were so severe that two of every three patients who entered the ICUs would ultimately die. In addition to training surgeons and caring for patients in the ICUs, I was tasked with repurposing non-medical space for the treatment of COVID-19 patients. This space was for patients who did not require intensive care. My hospital’s administration was familiar with my military experience and looked to me for solutions. I drew upon a decade of experience with the 1st Forward Surgical Team to assist with the redesign of any unused space. Conference rooms and lecture halls were rapidly reconfigured for patient care. When these spaces were exhausted, FEMA tents were set up for the overflow. By the peak of the pandemic, my hospital had almost doubled its capacity. As the command surgeon for the 353rd Civil Affairs Command (CACOM), I became very busy working with the command team to combat COVID-19 within the unit. Multiple soldiers had returned from Europe as travel restrictions were imposed and were rapidly dispersed to their homes across the U.S. Some of them began to show symptoms of COVID-19. Working through each state’s Department of Health requirements to obtain testing for soldiers was complicated. Recommending the closure and decontamination of a building after a soldier tested positive became necessary and served to complicate unit operations. It was my good fortune to have a commander and command staff that grasped the gravity of the situation and strove to ensure the safety of all soldiers. By March 25th, all unit activities were canceled and all activities were conducted virtually. In doing so, the chain of transmission within the 353rd CACOM was ended. As I write this on April 22nd, it has been reported that COVID-19 has peaked in New York. While this may be true, I can assure you that my hospital remains full of patients dying from infection with this virus. It is full of COVID-19 patients and all surge capacity remains open. Calls for the “rapid response team,” followed by “anesthesia stat” and sometimes by “code blue,” are hourly events. The crashing patients are rapidly transported to the ICU where critical care teams continue to wage a war against an unseen enemy. Time and distance will be required in order for scientists to develop the tools to defeat this deadly disease.
COL (Dr.) Omar S. Bholat
Distance Class of 2020
Command Surgeon, 353rd Civil Affairs Command (CACOM)